Social Research Projects
Our social research examines the effects of social stressors to better understand how they influence disease and to identify which of these stressors can be changed to improve health.
Projects overview
Our Study Populations form the basis for our research below:
Jump below to:
- Social adversities: the effects of socioeconomic status and discrimination on asthma risk and severity
- Allostatic load and asthma: the effects of social stressors on disease risk and severity
- Acculturation: the effects of acculturation on disease risk and severity
Social adversities
Social adversities are responsible for a large portion of poor health outcomes. Our research examines the effects of social stressors to better understand how they influence disease and to identify which of these stressors are amenable to targeted public health interventions which can improve health worldwide.
African Americans and Latinos have greater than twice the odds of living in poverty compared with whites. Low socioeconomic status (SES) is associated with high exposure to secondhand smoke, poor neighborhood and housing quality, increased exposure to violence, and decreased medication access, each of which is an important predictor of poor asthma outcomes. Social adversities negatively affect asthma by reducing access to asthma management and preventive medications.
These stressors increase the risk of asthma exacerbations and asthma susceptibility. According to the Life Course Health Development Model, “health is a consequence of multiple determinants operating in nested genetic, biological, behavioral, social, and economic contexts that change as a person develops” and chaos (defined as crowding, unpredictability, etc.) of the surrounding environment leads to deleterious health effects. In the context of one of our studies, the social stressors we experience over the life course increase the risk of asthma and modulate the course of asthma.
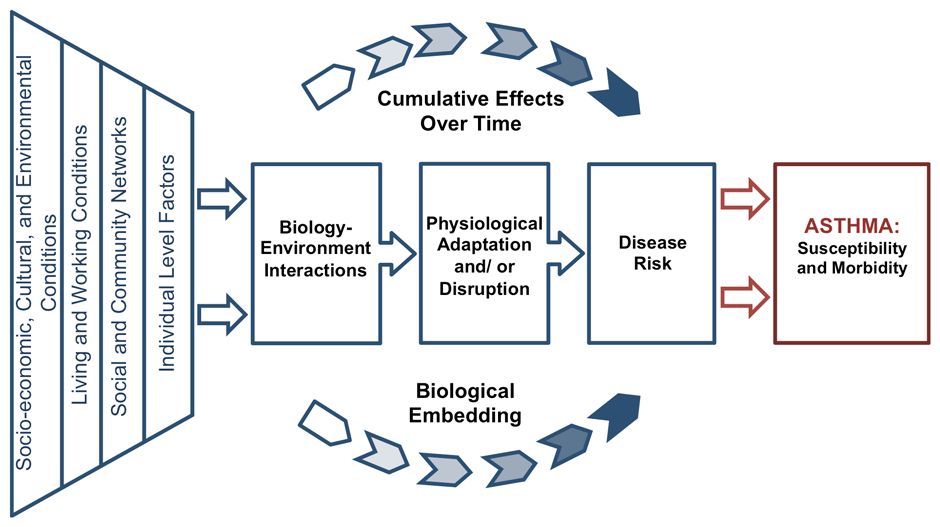
Health Model of Asthma and Social Adversities. Adapted from Lifecourse Health Development Model (Halfon, 2002) and the Toxic Stress Model (Center on the Developing Child, 2014).
We examined the relationship between socioeconomic status and asthma susceptibility through the study of 1,669 African American, Mexican American, and other Latino children with and without asthma. Using a composite socioeconomic index (SES index; range 4 to 8, with higher values indicating higher SES) derived from maternal educational level, annual household income, and type of medical insurance, we demonstrated that African American children had 23% greater odds of asthma with each decrease in the SES index (aOR1.23, 95%CI 1.09-1.38). Conversely, Mexican American children have a 17% reduction in the odds of asthma with each decrease in this index (aOR 0.83, 95%CI 0.72-0.96). Using the same SES index, we demonstrated that African American children with poor asthma control were more likely to be lower on the socioeconomic gradient (OR 1.17 for each unit decrease, 95%CI 1.05-1.32), and with the lower socioeconomic gradient there is a greater percentage of children with worse asthma control. This index was also associated with asthma-related symptoms, nocturnal awakenings, limitations of normal activity, and missed school days in our African American population.
Proportion of children with Controlled, Partially Controlled, and Poorly Controlled asthma along the composite socioeconomic index (P for trend = 0.005)
Children living in poverty are at high risk for obesity, which is associated with increased asthma morbidity and decreased drug response. We demonstrated that obese boys had 33% increased odds of worse asthma control than their normal weight counterparts (95% CI: 1.04-1.71). For girls this association varied with race/ethnicity. Obese African American girls (OR: 0.65; 95%CI: 0.41-1.05) were more likely to have better controlled asthma while obese Mexican American girls had a 1.91 (95%CI: 1.12-3.28) greater odds of worse asthma control when compared with their normal weight counterparts.
These results underscore the importance of studying both the effects of individual- and geographic-level social stressors and asthma. In addition, the differential response to social stress we reported emphasizes the need to examine these risk factors, and the mechanisms by which these stressors operate, in different racial/ethnic populations in order to reduce asthma prevalence and poor asthma outcomes.
Allostatic load and asthma
Minority children in the U.S. experience greater psychosocial stress than their white counterparts.
Increased psychosocial stress over the life course increases the risk for chronic diseases and worsens disease severity. In asthma, psychosocial stress may enhance airway inflammation via immunmodulation of cell function, thus affecting lung function and drug response. To better understand the role of social stressors on asthma, we have integrated the socio-ecological framework of the Life Course Health Development Model and the concept of allostatic load. Allostasis refers to the body’s ability to adapt to stress through activation of the sympathetic nervous system, the hypothalamus-pituitary-adrenal axis, and the metabolic system. As allostatic load increases, the “wear and tear” on the system leads to the dysregulation of stress hormones (epinephrine, norepinephrine, cortisol, etc.). In response, the metabolic and cardiovascular systems attempt to compensate, leading to disease or worsening of disease states. Individuals living in poverty carry a higher allostatic load and this may lead to an increase in asthma morbidity. We have created a conceptual model illustrating the role of allostatic load in asthma.
The role of allostatic load in asthma
Understanding allostatic load will allow for the development of targeted interventions that mitigate the impact of social stress on asthma. African Americans are more sensitive to stress, as illustrated by higher allostatic load than their counterparts, which leads to an increase in poor health outcomes. This differential effect may have important therapeutic implications, as populations with high allostatic load may have a blunted response to traditional asthma controller medications due to high circulation of stress hormones, which include cortisol. This response to stress is influenced by genetics, race/ethnicity, personal upbringing, and coping mechanisms. Given the rich data we have collected, we are able to explore the relationship between allostatic load, asthma outcomes, and social stress exposures in heterogeneous populations.
The total effect of an exposure (i.e., social stress) is the sum of the direct effect and the indirect effect. We hypothesize that allostatic load is a mediator in the social stress/asthma outcome pathway. We will use mediation analysis to estimate the effect of allostatic load on asthma susceptibility and asthma control.
Allostatic Load and Asthma: The total effect social stress on asthma outcomes is composed of the direct effect and the indirect effect (mediated Allostatic Load). Steps 1 through 3 assess association between the components joined by the dashed lines. Step 4 of the analysis determines whether the mediator mediates the exposure-outcome relationship.
Acculturation
Childhood asthma prevalence is rising in developed countries and disproportionately affects minority and economically-disadvantaged populations.
Latinos are a heterogeneous group comprised of a high proportion of immigrants and are traditionally thought of as an economically disadvantaged population. Asthma prevalence varies greatly across Latino subgroups, with Caribbean Spanish groups carrying the highest prevalence and Mexican Americans having one of the lowest prevalence, despite all groups having similar risk factors for poor health. Latinos are more likely to be uninsured or underinsured, resulting in limited access to regular health care. They are also more likely live in areas with high indoor and outdoor pollution exposure, and to be socioeconomically disadvantaged. Despite these risk factors, Latinos often have health outcomes similar to their non-Hispanic white counterparts. The “healthy immigrant effect,” cultural characteristics, and acculturation have been used to help explain the inconsistency. This “Hispanic Paradox” may explain the low asthma prevalence in Mexican Americans.
Acculturation is the process by which an individual adapts behaviors to reflect the dominant culture. It is related to the duration of time spent in the host country, as exposure to new risk factors for asthma increases over time. The place of birth and length of residence in the United States might influence early exposure to environmental factors that contribute to the development of chronic health problems. Several studies have demonstrated that low acculturation is associated with lower odds of asthma in Mexican Americans. The prevalence of asthma among Mexican Americans might therefore differ according to place of birth and changes in lifestyle associated with the acculturation process over several years of residence in the United States. There is a paucity of research in this area. Further understanding of the effects of acculturation on asthma susceptibility in Latino subgroups will allow for the identification of potentially at-risk groups who may have been overlooked, given the assumptions of the Hispanic Paradox.
Using the Genes-environments & Admixture in Latino Americans (GALA II) study we were able to show that acculturation imparts similar effects across several Latino subgroups, including Mexican Americans, Central and South Americans, and Other Latinos.
Acculturation. The odds of asthma among participants born in the United States compared with those who are foreign-born. Analysis adjusted for mother’s education, insurance status, age, sex, and history of breastfeeding.
